Here is a step-by-step explanation of how IV sedation is given. If you’d rather not know all the details and you’d like to find out about IV sedation for dental treatment, visit our IV sedation page instead!
IV is short for intravenous, meaning the drug is put into a vein. This is done using a cannula (commonly known as a Venflon) – a tiny flexible plastic tube which is placed into one of your veins in the back of your hand or in your arm.
One end sits inside the vein and the other end has a small valve that looks a bit like a tap (the blue bit). The drug is put in through this tap.
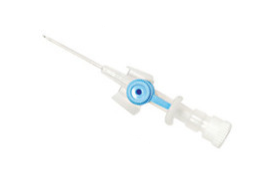
The venflon used for IV sedation in dentistry is usually one with a blue tap (like the one on the right, which still has its cap on).
How is the Venflon put in? – Step-by-step explanation
- The dentist or nurse checks your hands and arms to find the best place to put the Venflon. Tell them if you have a preference for where it goes. They might use a stretchy band around your arm to make your veins easier to see.
- Once you’ve decided on a suitable spot, you can put local anaesthetic cream on the area. Ametop cream is very effective! Local anaesthetic creams should be applied 30-45 minutes beforehand for maximum effect. The area stays numb for 4 to 6 hours. Alternatively, a topical cold spray just before putting in the Venflon can be used. You don’t have to use either of these if you prefer not to.
- The dentist or nurse will wipe off the anaesthetic cream and clean the area.
- A needle which is wrapped up with a tiny soft plastic tube (the Venflon) is inserted into the chosen site. The needle is then slid out, leaving the thin flexible tube in place.
- The Venflon is safely taped into place with a clear non-allergenic plaster or surgical tape, so it can’t accidentally get dislodged.
- Now the drug can be put in through the port (the blue bit).
- The Venflon stays in place from start to finish, so that the drug can be topped up as necessary and so that a reversal drug can be given if necessary (highly unlikely, but it’s reassuring to know that in the event of an emergency, a reversal drug or other emergency could be given).
Anything else?
Throughout the procedure, your pulse and oxygen saturation levels are measured using a pulse oximeter. This gadget clips onto a finger or an earlobe. It gives a useful early warning sign if you’re getting too low on oxygen, although if your dentist and the nurses are paying attention, they should see it way before the machine does!
Your blood pressure should also be checked, both before and after the procedure.
Back to What is IV sedation?