Dentists, psychologists and academics in Norway have a long track record of working together to bridge the gap between dentistry and psychology. Our DFC volunteer Nikoleta Gehrmann travelled to the Dental Faculty at the University of Oslo to find out more!
Lessons from Norway: dental fear management and trauma-informed care

Tiril Willumsen is a dentist and professor in Behavioural Science at the Dental Faculty, University of Oslo, Norway. Her primary research field is dental fear and psychologically traumatised patients in the dental clinic. She has a special interest in sexual abuse survivors and dental care, trauma-sensitive communication in the dental practice, and educating future dental personnel on the importance of these issues.
Anne Rønneberg is a PhD student and a Specialist in Paediatric Dentistry and Clinical Director at the Clinic for Child Oral Health Care, Faculty of Dentistry, University of Oslo. She has published several papers concerning child abuse in relation to dental treatment.
Ann Catrin Høyvik is a dentist with a BSc in psychology. She is a PhD student specialising in refugee oral health with a focus on dental fear and anxiety in torture survivors. She is also a dentist in private practice and teaches behavioural science to dental students.
Kjetil Strøm is a Specialist in Paediatric Dentistry. His PhD focuses on the use of behavioural management techniques for preventing and treating dental fear and anxiety in children and adolescents. He also teaches dental students and specialist candidates in paediatric dentistry and behavioural science at the University of Oslo.
Karianne Tveter and Marie Bjørnstad were 5th year undergraduate dental students at the University of Oslo at the time of the interview.
Nikoleta: Why is it that there is such a strong focus on dental fear and anxiety here at the Dental Faculty in Oslo?
Tiril: We started with behavioural sciences in about 1990. The woman who was the head of the faculty at that time decided that we needed a psychologist to hold a scientific position, and the faculty hired the one who became our first professor in social science and my supervisor. I am a dentist and I am also into behavioural science. Our focus is research and teaching students. We aim to enable students to prevent and treat dental fear and anxiety in patients using the most common sense approach possible. What I think is special about us is that very early on, we started to see dental fear and anxiety as a condition that may go beyond negative experience with a dentist when the patient was young. To see what’s behind the child that comes to the dentist. So we focus on traumatic experiences a lot, the child’s traumatic experiences and the window of tolerance, maybe you two students can tell something about this?
Karianne: Yes, in our studies we do a lot of behaviour management training. We do different kinds of exercises, like making a movie of ourselves talking to patients and training how to talk to them.
Marie: We have lectures about this from early on in our studies, and it’s always stressed how it’s really important to see the patient and not just the teeth. They always remind us that we have to be aware of the patient and how to communicate with them – both with trauma patients and also with patients in general to prevent them from developing anxiety.
Karianne: We try to explain everything we do. When we use the drill, we tell them what the drill does and if they are afraid, we ask them why they are afraid. Through explanations we try to prevent them from getting anxious.
Nikoleta: When exactly do you start with this training?
Marie: It starts in our fifth semester. We are with the medical students for the first two years and we start seeing patients in the sixth semester, so it’s the semester before we start seeing patients.
Tiril: It’s important to us to teach this aspect of dentistry before the students start with the clinic, so that they first learn to communicate and then they learn to drill. We’ve been lucky to have deans who think this is important.
Kjetil: They actually do start with behaviour sciences in the first month. To introduce them to dentistry, in the first couple of weeks we send them out to public clinics so they can see what it’s like to work as a dentist and how dentists treat their patients, what kind of patients they see, which kind of treatment they do. And, of course, if something happens during the consultations regarding dental fear, anxiety etc. After that we have a joint meeting in a group of eight people and I, Ann Catrin and Tiril answer any questions they may have and we discuss what happened, and we think about how it could be done better. Then at the beginning of the third year, we force them to role-play (laughs) the anxious patient and dentist, and we watch the recordings afterwards to see what they can do better and what they did well and give them tips. And we do the same later on in the same year.
The Four Habits Model
Nikoleta: Are there any special patient communication techniques you teach your students?
Tiril: Very much so – a method that is called “The Four Habits Model”.
Nikoleta: What is the technique about?
Ann Catrin: The four habits are: to invest in the beginning, to identify the patient’s perspective, to use empathy and to invest in the end of the consultation.
Tiril: This model should be used for the consultation as a whole, but also for each part of the consultation: during the anamnestic interview, during treatment, and after the dental treatment is finished. During dental treatment, you should explain what you will do (invest in the beginning), explore how this feels for the patient (identify patient’s perspective), show empathy and summarise afterwards: how was this for you, is there something you should do differently (invest in the end). So the four principles should be used all along the way. Besides, we of course focus on proper use of anaesthesia / analgesia, sedation, midazolam, benzodiazepine etc. and we also focus quite a lot on nitrous oxide sedation, so all students are also familiar with this.
Kjetil: We try to do it gradually so that they have the basics in medication, and then we get to patients with special needs like those who faint easily or where you can’t take x-rays because they’re gagging, also the use of different behavioural techniques and then, in the fourth year, we go on to the use of sedation techniques. In the last year, they learn more about treating more severe dental anxiety, so it’s about gradually increasing the level of difficulty.
Tiril: In the last year, we have a one-day seminar where we talk about traumatised children in the morning and traumatised adults in the afternoon. And in January we had a patient with us in a lecture who had been traumatised and she was talking about how she avoided dentistry for 15 years and how difficult it was for her with a very complex background. We focus quite a lot on childhood sexual abuse and other traumatising life events. Ann Catrin is writing her PhD about torture victims, who also have a complex background for their dental anxiety. We call it trauma-driven dental anxiety. We have a system in Norway that’s quite unique, psychologists and dental staff are working together in teams in special clinics all over the country. They treat traumatised people who have been sexually abused or been exposed to torture or have very serious dental anxiety.
Anne: At the students’ university clinic, we highlight that when people say they are afraid of going to the dentist, you have to ask questions – “How did you become afraid?”, “Can you tell me about it, why is it such a problem for you going through dental care?”. The patient does not answer every time, but you show that you care for them, you are opening the door when you ask “How did you become afraid?”, “Have you experienced something that you feel triggers you?”, some open-ended questions.
The Norwegian dental care system
Nikoleta: Can you tell me how the Norwegian dental care system works?
Tiril: Up to the age of 20 you have free dental care. From 18 to 20 it’s almost free. After that you are supposed to go to a private practice and pay all your expenses yourself. We have no general reimbursement for adults, but there is some reimbursement for parts of the treatment. And then we have some groups of patients who get all their dental care free, for instance those who have psychological impairments and people in institutions or in prison. In addition, the Norwegian government has established a treatment programme for dental treatment for persons exposed to torture, sexual abuse or who have a diagnosed dental phobia. It is called the TOO project. In this project, patients get both psychological treatment from psychologists and dental treatment from dentists, dental assistants and dental hygienists free of charge. This project is great, but we still need all dental personnel to be able to prevent anxiety from developing into phobia and to prevent patients to relapse into avoidance and phobia after TOO treatment.
Too many people lack coping skills during dental treatment, they avoid dental care and their anxiety increases. This is something that affects people‘s lives. I think it’s time for dental fear, anxiety and poor oral health to be highlighted as an oral, mental and general health problem. One of our struggles is therefore that what they call dental psychology should become part of the dental curriculum like endodontics, like periodontology. It’s a topic equal to those other topics, because if you don’t think about the psychology, you will lose those people who need treatment the most.
Ann Catrin: You have to see the whole person who is coming to see you, not just go for the teeth, that’s very important.
Marie: Proper communication skills are more than just being polite. Being polite might work for some patients, like those who are not afraid, but it won’t work for the patients who are afraid. And if you don’t know how to spot the difference, you’ll just be polite to everyone and it won’t work for some people.
Learning to work with phobic patients
Nikoleta: You’re in your last year of dental school right now – how prepared do you feel to work with phobic patients?
Karianne: That’s a hard question. I feel we have a good foundation, we know the theory and we know some things like how to expose the patient in small steps to be able to have treatment, but the more severe cases of anxiety are something I think I would refer or maybe I would call Tiril and ask. I think it’s that we don’t have the experience to say “this will work”. But we have the fundamentals, if that makes sense.
Tiril: This is something we have talked a lot about with Ann Catrin, she works in private practice besides doing her PhD. You need to be very skilled with the practical work.
Ann Catrin: Yes, it’s easier to work with really scared patients when you have a few years of clinical experience, because when I have to do a root canal treatment on a phobic patient, I have to be able to focus on the psychology and I have to carry out the dental treatment as quickly as possible. I think the more dental experience I get with the “normal” patients, the easier it will be to take care of the scared ones. It’s also difficult to meet a new dentally afraid patient and then the first thing I have to do is refer them to an endodontist and a surgeon. I have to be able to do some of the basic treatment first, so that’s why it’s even more difficult for young dentists.
Anne: We wrote an article about dentists’ self-perceived stress. The results showed that dentists with less than 10 years’ practice experienced more self-perceived stress and more difficulties when doing restorative treatment on children under the age of 10.
Tiril: We always say to dentists that they have to make time for dental anxiety. If you find four canals in a molar, you can’t say “I will only do root fillings on two of them because I don’t have time to treat the rest”. If you want to do your job properly, you must include this in your patient’s care because it’s so important.
Marie: It’s pretty time-consuming to treat phobic patients. It’s like, how willing are these patients to pay a bit extra to have the time to get rid of their anxiety? How do the patients respond if you tell them “you can pay a bit extra and we can put in more time”, so if you have more anxiety it might be more expensive than if you don’t have anxiety but how do the patients react…
Tiril: I think that many patients would react positively if you said that we can use extra time to make the situation less fear-provoking for them.
Ann Catrin: Yes, actually I do that a lot. Of course, there are people who don’t have the money at all for going to the dentist, and unfortunately people with less money often have more oral health problems. But a lot of people who have jobs and go to work and have a normal salary actually would like to pay a bit extra just for me to spend 15 extra minutes to take care of their psychological needs.
I am working with this patient now who has this gagging problem, and he is totally happy to pay whatever as long as we can take the time for him to relax and breathe. And it’s not that much, he goes to the dentist maybe twice a year and if he has to pay for an extra hour it’s no big problem. I think dentists are a bit afraid to ask, even though their patients may be perfectly OK with it.
Nikoleta: As students, do you sometimes feel afraid of nervous patients?
Marie: I had a patient when I was doing my internship. She had anxiety of going to the dentist but she needed to have a filling, so we started working and I remember she went into this state where her eyes were flickering and she appeared to be zoning out. We got back into contact with her, we went like “Hey, are you ok?” and she was like “Yeah, you can keep on going”, she was OK with us doing the treatment, but she said she was phobic. And we just took her hand and we said “You have to squeeze our hand so we know you’re still here with us”, and we got through it. So I think it’s not as scary as you might expect it to be, as long as you keep calm and communicate with the patient and just listen to what the patient is saying.
Ann Catrin: As a private practitioner, I think it’s well worth spending a bit of extra time on the first consultation with every patient anyway, scared or not scared. You invest that time, but it will save you so much time on all the subsequent appointments even with the scared ones, and also with patients who are a little bit demanding – those who are not scared, but just difficult in other ways. So if you invest in the beginning, everything that follows will go much more easily.
Ongoing research projects
Nikoleta: Tell me something about your research projects.
Kjetil: My project is about the use of behaviour management techniques when treating children and adolescents with dental fear and anxiety. My first paper was about public dentists’ use of different behaviour management techniques when treating children and how they felt about treating those patients. We found it quite interesting, because they used a lot of different behaviour management techniques but they didn’t use them as often as we would like. Also, those dentists who didn’t participate in postgraduate courses were using them far less than those who did. Only 50% of public dentists actually attend a postgraduate course on dental anxiety, which we thought was very low. Dentists should receive proper training. That’s one of the reasons why we are so focused on it here, because we have all heard the stories about public dentists who did massive fillings on our parents’ generation and we don’t want the new generations to repeat the tale, we want them to say “public dentists are good”.
Nikoleta: So this is one area of your research, are there any further topics?
Ann Catrin: I’ve been focusing on refugee oral health and dental fear in torture victims. Because we have always assumed that people who have been exposed to torture are afraid of going to dentist and also there have been some case reports, but there hadn’t been any systematic research. So I’ve been interviewing newly arrived refugees and doing oral health exams on them. I’ve been traveling to refugee centres and talking to and examining both torture victims and refugees with no torture experiences. We found that not all torture victims are afraid of going to the dentist, but a greater proportion than the non-torture refugees. The numbers maybe are not as high as expected, but the ones who are afraid are really at the top of the scale. So, there may be more non-afraid people than we thought, but those who need special treatment are really phobic. And also the ones who have experienced torture directed at the mouth are more afraid.
Now I’m doing a study with in-depth interviews with torture victims who have been to a dentist in Norway, so we try to figure out what they need, what they need us to do during treatment and how we should accommodate their needs.
Nikoleta: Do you have any initial ideas about how to help them?
Ann Catrin: Yes, we do, because there have been case studies. The most important thing for one of them was that the dentist and the staff were listening to them and were aware of their story and had time to care for them. Also, that the team was working well together, that they knew each other and respected each other and that they could feel that the nurse and the dentist were comfortable with each other. And it was important for them not to feel more pain than absolutely necessary and, needless to say, we have to know their story, because if they were exposed to waterboarding for example, then being tipped back and us going in with a lot of water – we really have to take care to use suction and remove the water and not give them the feeling that we are filling up their mouth with water.
But I think the most important thing is to recognise each patient and his or her story, because they all have different needs. It’s also important when they come back one year later that I remember that I shouldn’t shine the light right to their eyes or that I shouldn’t wear a white coat… small things, but I have to take notes for each patient so that next time when they come in I can have a look at the list of things that are important to her. The same goes for all afraid patients.
For some of people with torture experiences it’s difficult if there are too many people, so they may want to talk to the dental nurse first, but then they don’t want to have both me and the nurse over them – not for the first appointments at least. If I also have to use an interpreter and we are suddenly three people, you know, it would be this interrogation feeling that they have had before. It’s also very important for them to know what is going to happen because they have been exposed to being in prison and never knowing what is going to happen next. And also for some of them – and this is not only for torture patients but also for the some of the people who have been exposed to sexual abuse – sometimes it will be difficult to use sedation because they may feel that someone is going to do something that they have no control over. So that’s my project.
Tiril: We also have another interesting project, a collaboration between dentists and psychologists and social workers. We interviewed women and men exposed to sexual abuse as children. About half of them were regularly seeing a dentist and the other half of them were not. It’s a qualitative study, and the dentists focus on what the dental staff can do, the psychologists focus on how it feels to be in a dental practice for an abuse survivor, and the social worker has focused on how oral health and dental fear affect lives. It’s very interesting because the social worker is a very well known academic and she has a lot of experience with people with sexual abuse experiences. She had never thought about their oral health before, and she said “It’s so strange that we don’t think about that”. Because it was so important for the people we interviewed, oral health had such a huge impact. When you can’t smile, it really affects your life.
Anne: I’m writing up my doctoral thesis at the moment [spring 2019]. Our research showed that younger dentists are more stressed when treating fearful patients and children under the age of 10. We also found that the youngest dentists used conscious sedation more frequently than their older colleagues. Further we demonstrated that students with undergraduate education from Norway, compared to those educated from abroad, used less restraint when they had to carry out urgent dental treatment, for example when the child was in pain. We also studied how dental professionals and general professionals collaborate with child welfare services when they suspected child abuse. It’s very important because early intervention is crucial in child abuse, and we have to highlight it.
Kjetil: I think prevention is very important, it can’t be stated often enough. It’s important that all children attend the dental health care service and they should be met by an understanding dentist. Because when you see them as 60-year-old patients, the damage was done way earlier.
Sexual abuse and dental fear
Nikoleta: How did you get into the topic of childhood sexual abuse?
Tiril: The first time I had a patient that had been exposed to sexual abuse, it was very early in my research period and it was really tough for her and it emerged that she was about my age and lived near my home town. It was such a shock to me that this was something that was so close to me without me having any idea that this was going on. She had such hell at home and nobody knew what was going on. And then there was somebody who wrote in our national dental paper “why isn’t anybody concerned about us people who were exposed to sexual abuse and dentistry”, and I decided that I would do that. So I did this study back in 2001 involving women who were in self-help centres, and from that point on I’ve been passionate about this because it’s so difficult for them. I think dentists find it easier to avoid this subject, because it’s unpleasant to think about.
Nikoleta: What is different about abuse survivors and other nervous patients?
Tiril: I think it’s so much more complex. What needs to be done needs a different level of attention. Usually, when you have a simple fear, you are very scared of pain or being locked in, but with sexual abuse you are very afraid of being retraumatised, of having flashbacks, experiencing the trauma situation.
Ann Catrin: They get flashbacks, they have dissociation experiences in a different way from other phobics I think. I have a patient who sometimes, when she brushes her teeth, has a dissociative experience. She can get back to herself three hours later, she has trouble being on her own when brushing her teeth and that has to do with flashbacks… I don’t think this happens in the same way with people who haven’t been traumatised before. But then you have the people who have been traumatised by dental treatment also, they are also traumatised even if it hasn’t been sexual abuse, but they also feel traumatised so that’s a complex thing.
Tiril: Yes, and I think what’s more important than distinguishing between the two is to take the patient’s perspective. Each person has their anxiety, it’s very individual. The reason it has developed may be due to lots of things, some of them are conscious, some of them are unconscious. That’s why we focus on student education so much and on trauma-informed care, and that you should treat every patient as if they may be traumatised, and have some simple rules for making them feel safe. Don’t take their safety for granted. We shouldn’t think it’s obvious that they are safe with me.
The window of tolerance
Nikoleta: What are some of the rules for making someone feel safe?
Tiril: We work a lot with the “window of tolerance”.
Ketjil: Every patient has his or her window of tolerance. That means you can manage different things. And some have a very small window of tolerance, so if you go above or below that window they get overwhelmed.
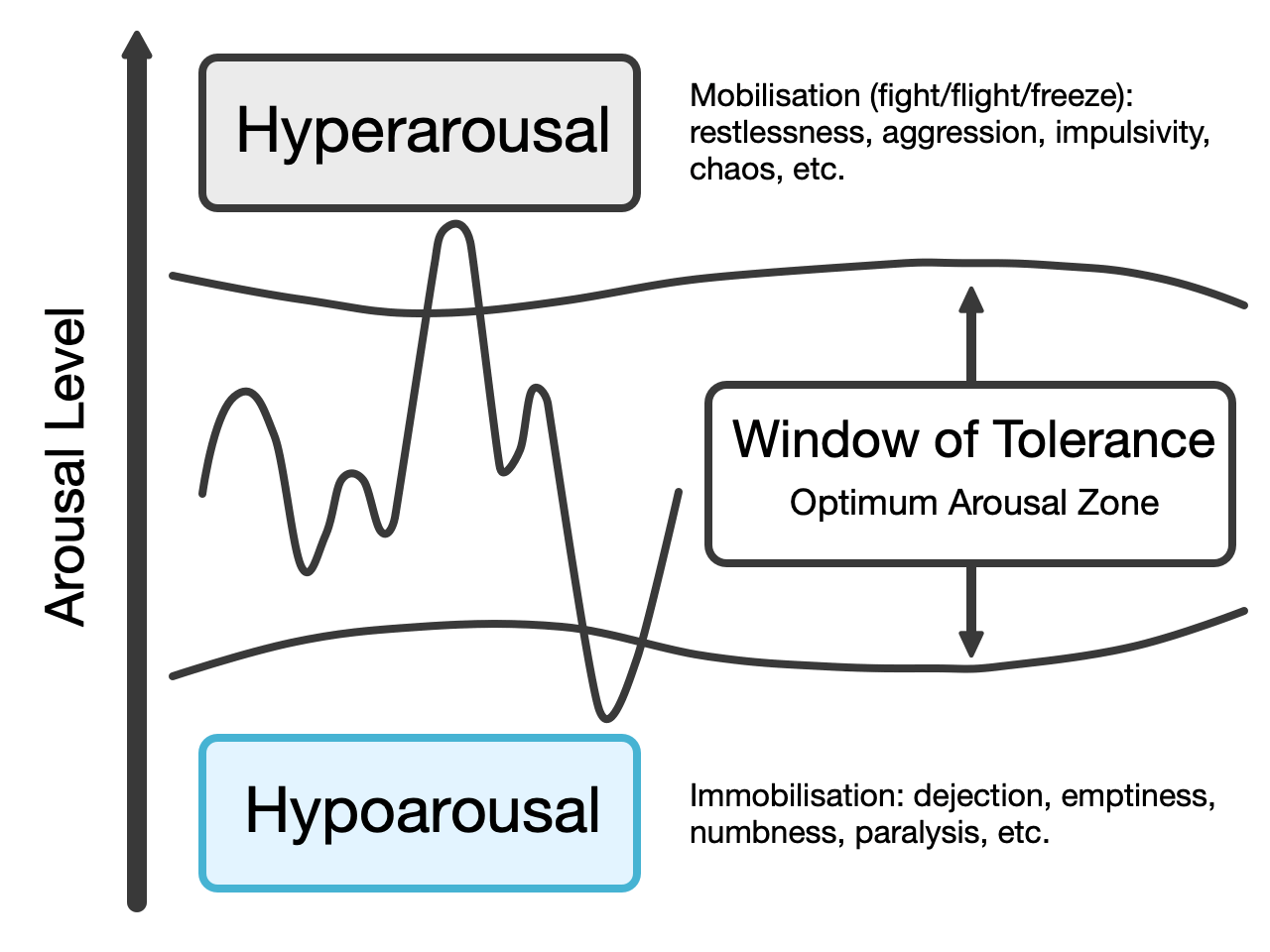
Ann Catrin: If you are below you are less active and also dissociating, you’re not able to do things, learn things, communicate, listen. But when you’re aroused too much it’s the opposite.
Anne: And this is the window you are comfortable with.
Ann Catrin: So if you are a psychologically healthy person, you will have a wide window of tolerance, things will happen and you won’t get stressed much, but if you’re traumatised, your window might be very narrow, so less distress is needed before you enter a state of hyperarousal or hypoarousal.
Ketjil: So if someone has been exposed to sexual abuse orally for example, they can react much more easy to like things like putting a finger on the side of the tooth or other small things that wouldn’t make another person dissociate. Another example is dissociating while brushing your teeth.
Tiril: Sometimes a person panics, everybody panics now and then, and we have coping strategies to get inside our tolerance window again and we know what to do. But a person who is traumatised will very often lack these coping strategies, so they stay in panic mode. And if you stay there, it’s so unpleasant that you can’t stand it. Then you just say goodbye to the world and you shut down and freeze. And eventually you learn these mechanisms. For example, if you’re traumatised as a child, you learn to do this during your abuse situations, and you use the same negative way of coping in the chair. So you have to be aware of this and if the patient is in a hyperaroused state, it’s necessary to calm them down. If they’re down you have to get them high – clap hands, remind them “You’re here, you’re with us, you’re at the dental office” and to wake them up. I am giving a lecture on this tomorrow to the second year students.
Ann Catrin: And maybe a problem for dentists who are not aware of this is that you always hear stories of people when the patient is underaroused, maybe resting with their eyes closed and the dentist thinks “OK, wow, the patient is great, now I can start working”. And they fill the whole quadrant or finish a lot of things at once and this will really retraumatise the patient and next time they will really just be worse.
Anne: And the window will get narrower.
Ann Catrin: We see this in torture victims who suffer from post-traumatic stress disorder, their tolerance window is really small, not only in dental situations but also in everyday situations. But they can work on this with psychologists and learn strategies to cope.
Anne: It’s very important for the practitioner to know about this window and talk to the patient about it, for helping them understand what is happening with them.
Ann Catrin: Every patient is different, one I am working with now I just have to keep her eyes open. Because we have been talking about that and I know once she starts to close her eyes she is dissociating. So I just have to go like “Hey, you have to open your eyes” and she then wakes up. Because if she’s been getting disconnected too much, then next time we meet it takes 20 minutes to get started instead of five.
The Anxiety Curve
Ann Catrin: We also use a concept called the “anxiety curve”. We explain to the patients what happens when anxiety is rising. When it rises above an acceptable level, you are so aroused that you might think that if you stay in the situation, the anxiety will just keep rising and rising and you will die. We explain to them that if you stay in the situation in a controlled way together with us, it will start to go down. Then we agree with them what their acceptable anxiety level is. For example, when we practice gradual exposure to needles, at first we might just sit with a needle lying on a table over there and look at it, and after maybe two minutes they see that “Oh, the anxiety is getting less”.
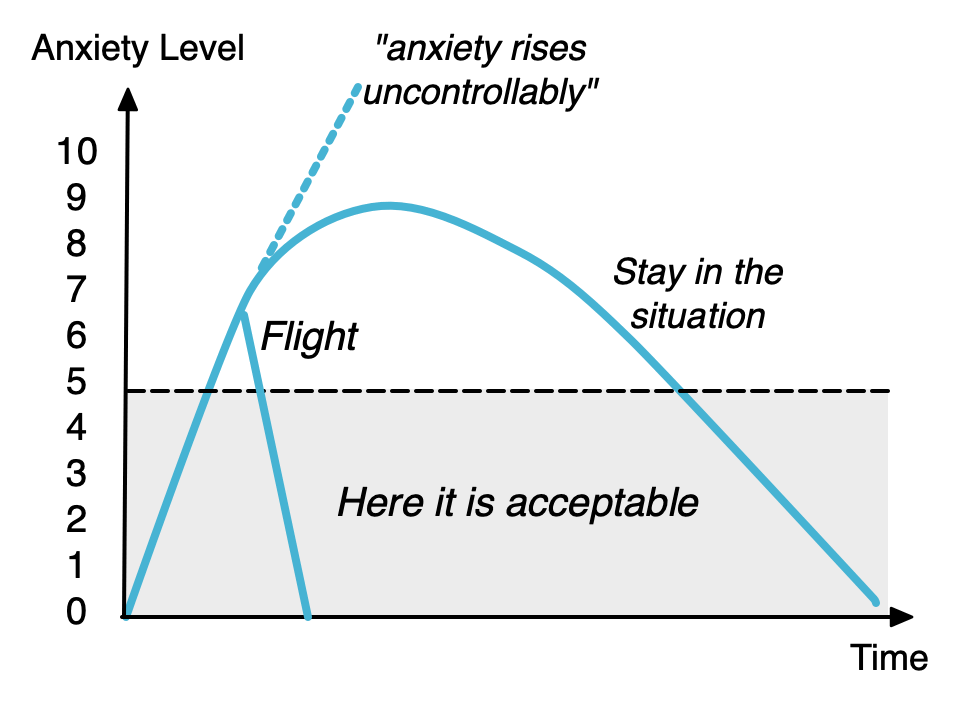
Kjetil: And you should always stay inside the comfort zone, because if you go too fast or you go to the edge, you panic or you freeze. You have to stay inside it.
Anne: We don’t start with the needle inside the mouth, we start where the patient is comfortable with it, and then take small steps closer and closer.
Kjetil: I also think if you want to practice holistically, you need to be able to offer several options for treatment, so here we don’t focus strictly on CBT as the only solution to dental fear. CBT is very effective, but it’s not always the best solution for everyone. As a paediatric dentist, I sometimes have patients who are motivated and able to have treatment, but who don’t have the cognitive abilities to actually see and do the exposure in the CBT treatment, and I think that’s sort of the start of the holistic approach because every patient is different.
Tiril: And this all has to be part of the dental curriculum. It has to be an equal part. When we have periodontal disease, you can’t do proper periodontal treatment without the patient being able to clean her teeth. And when it comes to dental fear, it is equally important to address the patients fears before you address the dental treatment. I think it’s quite comparable, because our goal should be to make enable people to keep their mouth healthy in the long run.
Date of Publication: 13 August 2020
You can read interviews with dentists who have an interest in helping nervous or phobic patients here