
Last updated on May 16, 2026
What can I do if the local anaesthetic doesn’t work?
Every time I go to the dentist, the local anaesthetic hardly does a thing for me, if at all, and I experience lots of pain at every visit, even for simple things like filling a cavity!
In the early days of the Dental Fear Central forum, we noticed a distressing issue coming up over and over again: people who were terrified because they had previously struggled to get numb. Realising how common this was, we reached out to several dentists who supported our website and message boards – including Mike Gow, Lincoln Hirst, and Fraser Hendrie – to ask for their advice on how people should handle this situation.
Their answers formed the original foundation of this very webpage. Here is a summary of their most important advice:
- You are in control: Never be afraid to ask for more anaesthetic (it isn’t expensive) or to halt the procedure and rebook if you don’t get profoundly numb. It is your mouth, and you have the final say!
- Find your “personal recipe”: Dentists have a huge array of tools, including multiple types of anaesthetic solutions, delivery methods, and injection sites. Tell your dentist in advance if you are hard to numb so they can dedicate the extra time needed to find the perfect combination for you. Once they discover your unique “recipe,” it will usually work every single time.1
- Seek out specific expertise: If standard techniques fail, look for highly experienced professionals. Dentists with a special interest in root canals (endodontists) or those who have worked in special care dentistry are trained experts in managing teeth that are difficult to numb.
Why can’t I get numb?
There are (without being alarmist – it’s a rare occurrence) a number of reasons why local anaesthesia may not work as well as it should do. The reasons are:
- poor technique
- unusual anatomy
- local infection (a “hot tooth”)
- some forms of Ehlers-Danlos syndrome
- your metabolism
- having red hair (?)
- hypersensitivity due to fear(?)
1. Poor technique (or choice of technique)
Some dentists are not very good at numbing but don’t think they have a problem or don’t care that they do. Most do care, but even the most experienced practitioner may not always be able to get you numb at the first attempt. Here are the reasons:
Not giving enough local anaesthetic
Sometimes it just takes some extra local anaesthetic to achieve profound numbing.
Not waiting long enough for the local to work
This is unlikely with modern local anaesthetics, but some people take longer to go numb than others. The solution is simply to wait until you are completely numb.
Placement of the local anaesthetic
The most common cause of not getting numb is when the dentist has missed the spot where they intended to put the local anaesthetic.
This problem usually arises when trying to numb lower teeth (especially lower back teeth) by blocking the nerve which supplies sensation to them. The usual technique for numbing lower back teeth is called the “inferior alveolar nerve block”. It should make your lips numb right to the midline. If it’s not working, often all it takes is trying again and putting the local into a slightly different spot.
But some people have unusual anatomy (see below). So if the inferior alveolar nerve block doesn’t do the trick, your dentist may be able to use an alternative or supplemental numbing technique. One example is an intraligamental top-up with a Wand or similar. Other examples include the Akinosi or the Gow-Gates technique. Some of these are “advanced” techniques and not all dentists will have them in their repertoire.
Giving the local too fast
Some local anaesthesia techniques may not work as well if the local is administered too quickly.
Choice of local anaesthetic
The most common anaesthetic solution used nowadays (lidocaine with adrenaline – also known as lignocaine or xylocaine) works best for most situations. But some people may have a high resistance to a particular local anaesthetic. In that case, your dentist can use a different one (for example articaine).
2. Unusual Anatomy
It was once explained to me that there are a small number of people who either don’t respond to anaesthesia or have a wacky nerve structure that makes it hard to place the novocain etc. where it will work 100%. I have to think this is my case. The dentist who told me this is now deceased and I’m running out of new ones to go to. If you were in my position, what would you do?
Local anaesthetic is always effective if it is given in the right spot and has enough time to take effect. It blocks the nerve supply to the region to be treated, so you can’t feel pain. However, there is huge anatomical variation between people. And some people have such an unusual anatomy that the “standard” dental block for lower bottom teeth used by 99% of dentists doesn’t work (the inferior alveolar block mentioned above). 2
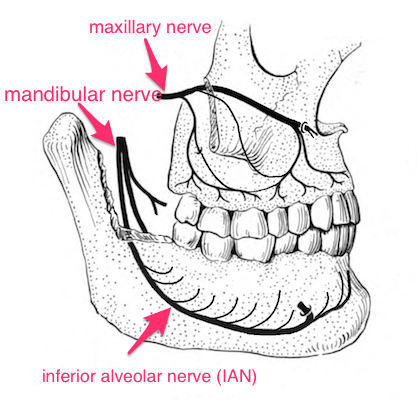
Unusual anatomy can be a particular problem with the lower jaw, because the dental nerve in the lower jaw is buried within dense bone. So giving local next to the tooth is usually not enough on its own to make that tooth completely numb. Instead, the main nerve which supplies sensation to that half of the jaw is numbed. This is done via an opening in the jawbone called the mandibular foramen.
The main reason why some people don’t go numb easily in the lower jaw is because the opening in their jawbone isn’t in the usual place. Everyone CAN be successfully numbed, but it may be necessary to use a different technique for numbing than the “standard” inferior dental block.
In contrast, the upper jaw is more porous (sponge like), so when anaesthetic is injected next to a tooth, it can get through to the root and make the tooth go numb.
Additional Nerves
It’s quite common to have some slightly unusual nerve connections. So in addition to the “usual” nerves, there may be additional or accessory nerves that supply the feeling for the tooth. When your dentist suspects that this is happening, you will need additional local in the right position.
For example, if you have trouble with upper back teeth not getting numb, a nerve called the greater palatine nerve can be the culprit. The solution is to give extra local in a different area to numb the accessory nerve.
Similarly, some people have accessory nerves in unusual places in the lower jaw. For example, there may be an accessory innervation of the lower teeth by the mylohyoid nerve. If you’re looking for detailed technical information, this article explains more: Four Common Mandibular Nerve Anomalies That Lead To Local Anesthesia Failures.
Again, there are always workarounds to these challenges, but you may need a dentist with a special interest in advanced local anaesthesia techniques. Read our tips on finding a dentist and email potential candidates to find out if they think they can help you!
3. Infection (“Hot Tooth”)
A raging localised infection (an acute abscess) can lessen the effectiveness of local anaesthetic. You can read more about abscesses on our root canal treatment page.
When there is an acute, painful abscess, the local anaesthetic may not work as well 3. Using more local anaesthetic (or using a different technique) usually does the trick:
It’s very very rare for a tooth to be so acutely infected that local won’t work properly. Usually, you can get around it by either putting more local in or else using a block injection to freeze the entire quarter of the mouth rather than just around the tooth. – Gordon Laurie, BDS
Another option is to postpone the root canal treatment or extraction needed to permanently sort the problem, and bring the acute infection under control first, using antibiotics.
N.B.: The signs of acute infection are heat, redness and severe pain. If you have an abscess and you don’t have these symptoms, you have a chronic abscess. In that case, ignore the above – the local anaesthetic will work as normal, and there’s no indication for antibiotics.
What do I do if the antibiotics don’t work?
Often your dentist will prescribe penicillins of some sort (e. g. amoxicillin), or an equivalent antibiotic if you’re allergic to penicillins. Usually, they’re very effective, but not always. These antibiotics kill off some bacteria, typically the aerobic (oxygen-breathing) bugs. But sometimes it can be necessary to kill off anaerobic bugs which contribute to the infection as well. A different antibiotic with an activity spectrum effective against anaerobes (such as Metronidazole) may help.
It may not always be possible to get rid of the infection completely, but it may have reduced enough to allow for comfortable treatment. If things don’t get any better (and you’re scared of trying again), you may want to look into sedation options, such as laughing gas or IV sedation.
With a painful abscess, the rule is to establish drainage. Opening up into the abscess through the tooth will produce almost immediate rapid relief of pain and can be better than waiting for up to 48 hours for antibiotics to have a noticeable effect. It’s not a painless method, but if you’re in unbearable pain anyway…
4. Ehlers-Danlos Syndrome
Ehlers-Danlos syndrome (EDS) is a group of rare genetic disorders which affect the connective tissues. Connective tissues include tissue such as skin, bone, organs and muscles. Symptoms may include joint hypermobility, easy bruising and stretchy skin. The symptoms can vary in severity and type, making each affected person’s case unique.
A major clinical trial in 2026 finally confirmed what many EDS patients have known for years: local anaesthetic may wear off much faster or fail more frequently for them 4. Prior to this, surveys had already highlighted the scale of the issue, with a 2019 study finding that a 88% of EDS patients reported past anaesthetic failure, compared to just 33% of the general population 5.
Researchers in the 2026 trial found that while the numbing agent (lidocaine) might work at first, it often leaves the system so quickly that patients are nearly three times more likely to experience anaesthetic failure during a procedure than the average person [1]. In fact, within just 30 minutes of an injection, nearly half of the EDS patients in the study were no longer fully numb. This suggests their bodies “clear” the medication out of the tissues at an accelerated rate, rather than being completely immune to the drug [1].
Tips from people with EDS
- Find a dentist who will actually listen!
- Explain that you have Ehlers-Danslos syndrome and that your body may metabolise or “wash away” the anaesthetic much faster than normal.
- Arrange a signal to give if the anaesthetic starts to wear off (I raise my hand).
- Ask for more frequent top-up injections rather than waiting for the pain to return.
- You may have better success with different types of anaesthetic, such as Articaine (Septocaine) or Carbocaine, which may have different durations of action.
- Don’t wander off and wait for it to take effect like in a “normal” patient – by the time the dentist returns the anaesthetic has often worn off.
- If there may be discomfort after a procedure, give another injection before sending the patient home.
- There are other EDS pointers for dentists – you need to be sure that your neck is supported during dental procedures. Your dentist should allow frequent breaks during prolonged treatment to avoid straining the ligaments of the jaw. Gums and tissues are fragile and bleed and tear easily. Sutures may not hold well.
5. Your metabolism
Your body’s biochemistry may be slightly different from that of the average person, and this may prevent the anaesthetic from working as expected. While most people are numb after 5 to 10 minutes, others take much longer to get numb. In some people, the anaesthetic wears off much faster than expected, whereas in others, it lasts much longer than expected.
The key is to find a solution together with your dentist – it just takes some extra time and a bit of trial and error.
6. Having Red Hair (?)

If you are a natural redhead and have ever felt that dental numbing doesn’t work as well for you, you are not alone – and it is certainly not “all in your head.” People with red hair often seem to need a little extra help getting completely comfortable in the chair.
The biological culprit seems to be a mutation in the MC1R gene 6. This is the gene responsible for giving you red hair and fair skin, but it has a fascinating secondary role: it also affects the receptors in your brain and central nervous system that process pain.
Why You Might Still Feel Something
In the past, scientific studies seemed to contradict each other. Some research showed redheads needed more anaesthetic 6, while other studies proved the numbing injections blocked the nerves just as successfully in redheads as anyone else 7.
Today, we understand that both things can be true at once.
Because of the MC1R gene, your nervous system may process physical sensations more intensely 8. Even when a local anaesthetic successfully blocks the main nerve from feeling traditional pain 7, your brain may remain highly receptive to other stimuli. This means that while you are technically numb, your nervous system may still intensely pick up on the cold water or the strong vibration of the dental drill – and it can easily interpret those intense feelings as sharp discomfort 8.
What this means for your dental visits:
Top-ups are completely normal: Because of this genetic sensitivity, you might simply need a slightly larger initial dose or a quick “top-up” during the procedure. Any good dentist will be more than happy to adjust for you.
Trust your body: You are not “immune” to the medication, but your genetic makeup means you are naturally more sensitive to the physical sensations of dental work. If you feel uncomfortable, your experience is valid.
Give your dentist a heads-up: You don’t need a medical diagnosis; simply say that from past experience, you need more local anaesthetic than the standard dose.
7. Anxiety (?)
It’s been suggested that when someone is highly stressed or anxious, the local anaesthetic may not work as well as when you’re relaxed. The local anaesthetic may not kick in as quickly, it may not be as effective, or it may wear off too quickly.
We don’t know whether this theory is true or not. Most people with high levels of anxiety get numb without a problem. Or they usually get numb in one location, and not in another. It may be that people who have experienced inadequate numbing in the past are understandably very anxious. And when the numbing fails again, this is interpreted as their anxiety causing the anaesthetic to fail – when the real reason might be anatomical variation, poor technique, or individual differences in metabolism.
Also, since nearly all people experience at least some degree of anxiety during dental treatment (and 48% of people in the UK have moderate to severe levels of dental anxiety)9, it is nearly always possible to attribute incomplete numbing to anxiety.
Sedation and Pain Perception
Whatever the reason for not getting numb may be, sedation (either nitrous oxide or IV sedation) can help with altering the perception of pain. People seem to react to stimuli differently when sedated, and for some people, this makes all the difference.
So sedation is well worth considering if you repeatedly don’t get numb with different clinicians. You will be able to communicate with your dentist when using conscious sedation. This means that you can stop immediately if you are not numb enough using a pre-agreed stop signal (though often, dentists will pick up on any signs of discomfort before you’ll get a chance to use it).
Visit our support forum to get help with this and other fears, or to simply get things off your chest!
You may also like:
- Is tooth numbing an all-or-nothing phenomenon?
- Intraosseous injection – success!
- Feeling fleeting moments of a chilling gnawing sensation during drilling
- Failure to numb lower jaw
- Incomplete numbing – would a CBCT or MRI scan be useful?
- What is an intraosseous injection like?
- Success
Further Reading
- How to overcome failed local anaesthesia by J.G. Meechan (PDF file) (***trigger warning*** – very explicit images)
- Four Common Mandibular Nerve Anomalies That Lead To Local Anesthesia Failures
Footnotes and Sources of Information
- On this page, we mention some examples of more advanced dental injection techniques. Although the “standard” numbing techniques work most of the time for most people, numbing teeth isn’t just a case of putting local anaesthetic next to the tooth to be numbed. It’s a bit more complex: (a) there are a variety of numbing techniques which work by numbing a single tooth; (b) other numbing techniques involve numbing the nerve or nerves which supplies sensation to a group of teeth. Again, there are a variety of these technique; (c) it may also be necessary to numb so-called “accessory nerves” which may supply sensation to certain teeth; (d) the anatomy and nerves are different for the lower and the upper jaw; (e) some injection techniques are suitable for some teeth but not others – it depends on which tooth it is (e. g. a front tooth, a back tooth, upper jaw, lower jaw, etc.).[↩]
- Four Common Mandibular Nerve Anomalies That Lead To Local Anesthesia Failures. James L. Desantis, DDS, M.D., and Charles Liebow, DMD, Ph.D. (2014). Chairside Magazine Volume 9, Issue 2.[↩]
- Ueno, T., Tsuchiya, H., Mizogami, M., & Takakura, K. (2008). Local anesthetic failure associated with inflammation: verification of the acidosis mechanism and the hypothetic participation of inflammatory peroxynitrite. Journal of inflammation research, 1, 41–48. https://doi.org/10.2147/jir.s3982[↩]
- Bourne KM, et al. Patients with Ehlers-Danlos syndrome experience reduced effectiveness of lidocaine local anesthetic: a randomized cross-over clinical trial. Regional Anesthesia & Pain Medicine. 2026. https://doi.org/10.1136/rapm-2025-107416[↩]
- Schubart JR, Schaefer E, Janicki P, Adhikary SD, Schilling A, Hakim AJ, Bascom R, Francomano CA, Raj SR. Resistance to local anesthesia in people with the Ehlers-Danlos Syndromes presenting for dental surgery. Journal of Dental Anesthesia and Pain Medicine. 2019;19(5):261-270. https://doi.org/10.17245/jdapm.2019.19.5.261[↩]
- Liem EB, Lin CM, Suleman MI, Doufas AG, Gregg RG, Veauthier JM, et al. Anesthetic requirement is increased in redheads. Anesthesiology. 2004;101(2):279-283. https://doi.org/10.1097/00000542-200408000-00006[↩][↩]
- Droll B, Drum M, Nusstein J, Reader A, Beck M. Anesthetic efficacy of the inferior alveolar nerve block in red-haired women. Journal of Endodontics. 2012;38(12):1564-1569. https://doi.org/10.1016/j.joen.2012.08.014[↩][↩]
- Liem EB, Joiner TV, Tsueda K, Sessler DI. Increased sensitivity to thermal pain and reduced subcutaneous lidocaine efficacy in redheads. Anesthesiology. 2005;102(3):509-514. https://doi.org/10.1097/00000542-200503000-00006[↩][↩]
- NHS Information Centre for Health and Social Care: Adult Dental Health Survey 2009.[↩]