
Last updated on January 17, 2021
Pain in the jaw, the jaw joint, and the surrounding muscles is known as TMJ pain. TMJ is short for temporomandibular joint (or jaw joint in plain English). Problems that affect the jaw joint are known as TMDs (temporomandibular disorders). It is a common condition.1
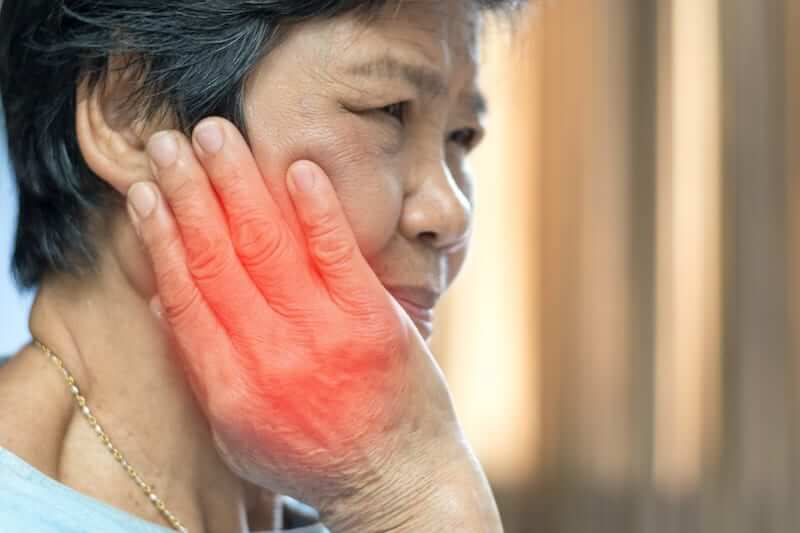
What causes TMJ pain?
It’s often hard to know what exactly is causing TMD. Genetics and anatomy can play a part. Sometimes the cause is obvious, such as an injury from a heavy blow. Other causes can include arthritis and wear and tear of the joint.
But most of the time, the pain is a bit of a mystery. Clenching or grinding the teeth is a common culprit (although not everyone who clenches and grinds gets TMJ pain). The challenge is that it tends to happen during sleep, so people aren’t aware of it.
Unfortunately, clenching and grinding puts a lot of pressure on the jaw joint, the muscles, or even the teeth, often for hours on end. This can completely overload the system and cause pain or other symptoms such as headaches. Believe it or not, ideally, the teeth should only touch between 4-10 minutes in the day whilst eating or speaking!
Because so many different factors can contribute to TMD, there is no easy cure. Luckily, we do know of a few things that can help with the symptoms.
What can help with TMJ pain?
Most of the time, TMJ pain goes away on its own after several weeks or months. We know that stress has a strong link to TMD but it’s almost impossible to remove all sources of stress in your life (if you find out how to please let us know!).
The tips and advice included below can help reduce the stress on the jaw, the muscles, and the teeth, encouraging the healing process. More often than not a simple approach is enough to settle the pain, so it makes total sense to do the simple things first before considering anything more invasive (or costly!).
1. De-stress

Do something that relaxes you and lowers your stress levels, for example:
- go for a walk (especially in nature)
- meditation, yoga, or mindfulness
- relaxation techniques
- exercise
- play a video game
- have a relaxing bath
- play an instrument, paint, do arts and crafts or baking
- listen to music.
Often, it can be more helpful to tackle the cause of the grinding rather than manage the after-effects. Unconscious habits such as clenching or grinding may stop when the source of stress or anxiety is removed. If you like, speak to your GP who may refer you to a psychologist or cognitive behavioural therapist for additional support.
For clenching or grinding during the night, it’s best to do some form of relaxation just before going to sleep. For example, you could listen to guided meditations or self-hypnosis tracks (check out apps such as “Calm” or the mp3 further down under “Hypnosis”).
2. Eat differently
If you eat food that doesn’t require lots of chewing, your jaw gets a chance to rest and heal.

Here are some tips:
- Don’t take big bites and don’t open your mouth too wide
- Try not to use a grinding side-to-side motion
- Cut your food up into small pieces
- Avoid chewing gum and ice (and other hard foods)
- You may want to switch to soft foods for a few weeks and see if that helps: Soft Food Ideas
3. Ice packs, heat, and massage
Moist heat
A steamed towel can help loosen up tight muscles. Or boil some water, soak a washcloth, then wring it out and place it into a ziplock bag. That way it won’t drip and it will retain the heat longer. Hold it to the side of your face and temple for about 10 to 15 minutes.

Ice packs
Apply ice packs to the side of your face for about 5 minutes. A bag of frozen peas is good, wrapped in a tea towel. Ice packs can help with inflammation and swelling and numb the pain.
Heat and massage
Applying a hot water bottle or hot pack and massaging the area may help, too. If you are the crafty type, you can make rice packs, where you sew a little cotton bag and put rice in them. They can be heated in the microwave and the heat lasts for quite a while.
I started this thing where I wet a washcloth with hot water (as warm as I can stand) and hold it on/below my ear and around my jaw for 15 minutes, then switch to an ice pack for 15, then alternate back and forth for an hour or two. Sometimes I only use the warm washcloth. It helps just enough to loosen the jaw so I can massage it until it sort of “clicks” back into a better position to where it doesn’t hurt as much. Not sure if it will work for everyone, but it definitely helps me. – from our message boards
4. Splints and night guards
Splints fit over teeth and prevent the upper and lower teeth from coming together.
Over-the-counter night guards are available in drug stores. DIY guards aren’t great but can be used as a sort of diagnostic device: if you use one and things get better, then it’s probably worth getting a proper one made.
But ideally, ask your dentist for a custom-made one. Stabilisation splints (also called Michigan or Tanner splints) are generally accepted as being the most effective. Splints give your jaw joints and muscles a chance to relax and heal, and they also discourage clenching.
5. Physiotherapy
Some of our forum members have found relief from visiting a physiotherapist with an interest in treating TMJ. Physiotherapy can be especially useful for tender muscles, neck or back pain, or limited opening of the jaw. Physiotherapists can also work on improving posture, another factor that contributes to TMD.
You can also ask your dentist if they can recommend any gentle stretching exercises you can do.
6. Medicine
Depending on the cause of the symptoms, these medications may help relieve TMJ pain:
Painkillers: Being in constant discomfort can make pain worse, which can further increase our stress levels. So it can be a good idea to take over-the-counter pain relief. The top choices are ibuprofen, paracetamol, and aspirin. Check with your pharmacist that you can take them.
Topical creams: Creams or gels such as Theraflex or Arnica cream may also help.
Botox: Botox can reduce muscle activity, and appeals to those who cannot face wearing a splint at night.
Muscle relaxants: Occasionally, these are used for a short period of time to help relieve TMJ pain caused by muscle spams.
Tricyclic antidepressants such as amitriptyline: These are usually used for depression. But there is some evidence that low doses may reduce the pain of chronic TMD. 23. As medications can have side effects, you should try other options first.
7. Hypnosis
Hypnosis can be really helpful for reducing or even stopping clenching or grinding (and lowering stress levels more generally). Make sure you see a qualified hypnotherapist. If you are in the UK, that would be someone who is registered with one of the major UK hypnosis societies, such as BSECH, BSMDH, BSMDH (Scotland), BSMDH Mets & South, or RSM Section of Hypnosis & Psychosomatic Medicine.
You can also listen to hypnosis mp3 recordings for clenching and grinding. Like other relaxation methods, these may be especially helpful before bed. Mike Gow, who’s on our advisory board, has produced a 60-minute mp3 which can be bought on eBay. Search for “Stop clenching & grinding your teeth: Managing bruxism with Dr Mike Gow”.
8. Other tips for reducing TMJ pain
Here are some more tips which may help reduce TMJ pain:

- Keep your teeth slightly apart as often as you can
- Avoid opening your mouth wide – that includes singing and yelling
- When it’s cold outside, wrap a scarf around your neck and generally dress warmly (cold will make your muscles tense up and increase discomfort)
- Put your hand under your chin when yawning to keep it from opening too wide
- Avoid habits such as nail-biting
- Sleep on your back, not on your stomach
- Sit and stand straight, and don’t hunch over
- Don’t hold the phone between your shoulder and ear
- Don’t rest your chin on your hand
9. Seeing a TMD specialist (?)
This is a difficult one. Because in a lot of cases, nobody really knows for sure why TMJ pain occurs and how to cure it, there are a lot of quacks around who promise relief. TMJ can come and go for no apparent reason, so some quacks will simply get lucky with the timing, resulting in an apparent “cure” (which would have happened anyway).
Perhaps the most notorious example is “neuromuscular dentistry” (LVI), which can involve crowning lots of teeth that don’t need any treatment for vast amounts of money.
We’ve also had people on our forum being quoted thousands of dollars for a splint by self-proclaimed TMD experts.
If the tips on this page don’t bring relief and you’d like to seek out someone with extensive expert knowledge on TMD, you can look for
- specialist oral maxillofacial surgeons
- dentists with additional training in orofacial pain (but see the caveats above).
The most reliable way of finding a reputable TMD practitioner is via a good dentist who may know of one or who may be able to find out from colleagues.
Find out how to recognise a good dentist!
You could also ask your GP for a referral to a specialist pain clinic. In addition to providing help with the physical side of pain, they can offer psychological support and tend to take a very rounded approach to pain management. There may be long waiting times in some parts of the UK, though.
10. Surgery
It is very rare to use surgery for TMD. But it can be suggested as a last resort when nothing else helps. If a doctor suggests surgery, be sure to discuss all the potential risks and benefits and ask what all your options are. You may also want to get several opinions.
You can find more information about surgical and other procedures (including arthrocentesis, which is a minimally invasive procedure) on the Mayo Clinic website: TMJ disorders
Further Reading
The Curious History of Occlusion in Dentistry by Dr. Barry Glassman and Dr. Don Malizia
You may also like:
Sources of Information
- National Institute of Dental and Craniofacial Research: Prevalence of TMJD and its Signs and Symptoms[↩]
- Rizzatti-Barbosa CM, Nogueira MT, de Andrade ED, Ambrosano GM, de Barbosa JR. Clinical evaluation of amitriptyline for the control of chronic pain caused by temporomandibular joint disorders. Cranio. 2003. Jul;21(3):221–5. 10.1080/08869634.2003.11746254[↩]
- Alajbeg IZ, Boric Brakus R, Brakus I. Comparison of amitriptyline with stabilization splint and placebo in chronic TMD patients: a pilot study. Acta Stomatol Croat. 2018;52(2):114-122. doi:10.15644/asc52/2/4[↩]